
Roy A. Rothman, DPM, PA
Podiatric Medicine and SurgeonFoot & Ankle Specialist


Heel pain can be difficult to deal with, especially if you do not know what the underlying cause is. If you ignore your heel pain, the pain can magnify and potentially develop into a chronic condition. Depending on the location of your heel pain, you have developed a specific condition.
One condition is plantar fasciitis. Plantar fasciitis is caused by the inflammation of the plantar fascia, or the band of tissue that connects the heel bone to the base of the toes. The pain from this condition is initially mild but can intensify as more steps are taken when you wake up in the morning. To treat this condition, medication will likely be necessary. Plantar fasciitis is often associated with heel spurs; both require rest and special stretching exercises.
There are various options your podiatrist may suggest for heel pain. Treatment options for heel pain typically include non-steroidal anti-inflammatory drugs (NSAIDS), which may reduce swelling and pain. Other options are physical therapy, athletic taping, and orthotics. In severe cases of heel pain, surgery may be required.
Preventing heel pain is possible. If you are looking to prevent heel pain from developing in the future, be sure to wear shoes that fit you properly and do not have worn down heels or soles. Be sure to warm up properly before participating in strenuous activities or sports that place a lot of a stress on the heels. If you are experiencing any form of heel pain, speak with your podiatrist to determine the underlying cause and receive the treatment you need.
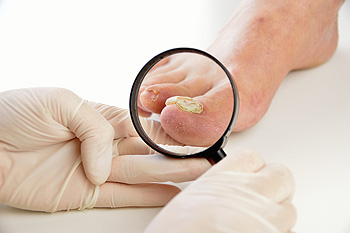 Fungal nail infections, also known as onychomycosis, can cause the nails to become thick, yellow, and crumbly. Fungal nail infections are usually not painful unless they become severe. Small cracks in the nail or the skin surrounding the nail allow for fungi to come into the nail and infect it. Those who have an injury to the nail, are diabetic, or have a weakened immune system, are said to be at a higher risk of developing a fungal nail infection. Fungi often thrive in warm, moist environments, such as locker rooms and public pools, and the fungi tend to spread to others while in these areas. Because antifungal medication or removal of the nail may be necessary to get rid of the infection fully, those who are experiencing a fungal nail infection should consult a podiatrist.
Fungal nail infections, also known as onychomycosis, can cause the nails to become thick, yellow, and crumbly. Fungal nail infections are usually not painful unless they become severe. Small cracks in the nail or the skin surrounding the nail allow for fungi to come into the nail and infect it. Those who have an injury to the nail, are diabetic, or have a weakened immune system, are said to be at a higher risk of developing a fungal nail infection. Fungi often thrive in warm, moist environments, such as locker rooms and public pools, and the fungi tend to spread to others while in these areas. Because antifungal medication or removal of the nail may be necessary to get rid of the infection fully, those who are experiencing a fungal nail infection should consult a podiatrist.
For more information about treatment, contact Roy Rothman, DPM of Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please feel free to contact our office located in DeBary, FL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Fungal infection of the toenail, or onychomycosis, typically appears as a gradual change in a toenail’s texture and color that involves brittleness and darkening. The fungal infection itself occurs beneath the surface of the nail. Aside from discoloration, other symptoms include the collection of debris beneath the nail plate, white marks on the nail plate, and a foul odor emanating from the nail. If ignored, the infection can spread into other nails and the skin; in severe cases, it can hinder one’s ability to work or walk.
The toenails are particularly vulnerable to contracting infection in moist environments where people are likely to be walking barefoot, such as around swimming pools, public showers, and locker rooms. Fungal infection may also be more likely to occur in nail beds that have been injured, and sufferers of chronic diseases such as diabetes, circulatory problems, or immunodeficiency conditions are particularly prone to developing fungal nails.
Fungal nails can be primarily prevented by practicing proper hygiene and regularly examining the feet and toes. Carefully washing the feet with soap and water and thoroughly drying the feet afterwards are essential. Other tips include wearing shower shoes in public areas, changing shoes and socks daily, keeping toenails clipped at a short length, wearing breathable shoes that fit properly, wearing moisture-wicking socks, and disinfecting home pedicure tools and instruments used to cut nails.
Fungal nail treatment may vary between patients and the severity of the condition. Your podiatrist may suggest a daily routine of cleansing that spans over a period of time to ease mild infections. Over-the-counter or prescription antifungal agents may also be prescribed, including topical and/or oral medications. Debridement, or the removal of diseased nail matter and debris, may also be performed. In more severe cases, surgical treatment may be needed. In some instances, the temporary removal of the fungal nail allows for the direct application of a topical antifungal to the nail bed. In other cases, a chronically painful fungal nail that has not responded to other treatments may be permanently removed; this allows the infection to be cured and avoids the growth of a deformed nail.
 Prior to choosing the right running shoe for you, there are several important factors to consider. One of these is the pronation of your foot. Pronation refers to the rolling of the foot from the heel to the toe when your foot strikes the ground while you walk. Ideally, your foot should strike the ground with the outside of the heel and move up to the ball of your foot evenly. People who have overpronation roll the foot too much towards the inside while they walk. People who have underpronation roll the foot too much to the outside while walking. Your gait pattern can help determine what the best running shoe for you looks like. For example, if you have overpronation, you may want to opt for a shoe that offers motion control and stability. For more information on how to pick the best running shoes for you, consult with a podiatrist today.
Prior to choosing the right running shoe for you, there are several important factors to consider. One of these is the pronation of your foot. Pronation refers to the rolling of the foot from the heel to the toe when your foot strikes the ground while you walk. Ideally, your foot should strike the ground with the outside of the heel and move up to the ball of your foot evenly. People who have overpronation roll the foot too much towards the inside while they walk. People who have underpronation roll the foot too much to the outside while walking. Your gait pattern can help determine what the best running shoe for you looks like. For example, if you have overpronation, you may want to opt for a shoe that offers motion control and stability. For more information on how to pick the best running shoes for you, consult with a podiatrist today.
If you are a runner, wearing the right running shoe is essential. For more information, contact Roy Rothman, DPM from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Choosing the Right Running Shoe for Your Foot Type
To increase performance and avoid the risk of injury, it is important to choose the right running shoe based on your foot type. The general design of running shoes revolves around pronation, which is how the ankle rolls from outside to inside when the foot strikes the ground.
If you have any questions please feel free to contact our office located in DeBary, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Running may seem like a simple to do. However, running is actually a complex movement that puts stress on the ligaments, bones, and joints of the body. Selecting the correct running shoe is important for increasing performance and avoiding risk of injury. Running shoes should be selected based on your foot type. Considerations such as trail versus road shoes are important. Your foot type dictates the degree of cushioning, stability and motion control you require. The most accurate way to learn your foot type is to visit a local shop that specializes in running shoes. Professionals can measure your arch type, stride and gait and help you with your shoe needs.
The design of running shoes is created around the idea of pronation. Pronation is the natural rolling movement of your ankle from the outside to inside when your foot strikes the ground. If you run properly you strike the ground on the outside of your heel and roll in the direction of your big toe before pushing off once more. Pronation is beneficial because it assists the lower half of your body in absorbing shock and storing energy. Those considered neutral runners pronate correctly and do not need running shoes that help correct their form. Neutral runners can choose from a wide variety of shoes, including barefoot or minimal types. However, those who have arch problems or who adopt an incorrect form while running may experience too much or too little pronation. They may require running shoes that offer additional support.
Those who overpronate experience an over-abundance of ankle rolling. Even while standing, those who severely overpronate display ankles that are angled inward. It is not uncommon for them to have flat feet or curved legs. The tendency to overpronate may cause many injuries. Areas that tend to become injured are the knees, ankles, and Achilles tendon. If you find that you have a tendency to overpronate, you should look at shoes that provide extra stability and motion-control. Motion-control shoes are straight and firm. Shoes of this type do not curve at the tip. The restricted flexibility along the middle of the shoe prohibits the foot from rolling too far inward as your foot strikes the ground.
A less common problem is underpronation. Underpronation, also called supination, is when the feet are unable to roll inward during landing. Those who underpronate have feet that lack flexibility and high arches. This prevents any kind of shock absorption, even though it does place less rotational stress on ankles and knees. This added force can cause fractures, ligament tears, and muscle strains because the legs are trying to compensate for the impact. Those who underpronate need shoes with more cushioning and flexibility. If you have a tendency to underpronate, selecting stability or motion-control shoes may cause you more problems by continuing to prevent pronation.
 The pain and discomfort that is found in plantar fasciitis is located in the heel and arch area of the foot. It develops as a result of inflammation that affects the plantar fascia. The plantar fascia is a band of tissue that connects the heel to the toes and runs along the bottom of the foot. The contributing factors for developing plantar fasciitis can include standing on hard surfaces for the majority of the day and wearing uncomfortable shoes, such as high heels. Additionally, patients who have gained weight may develop this ailment, and it can affect people who have low or high arches. The pain that accompanies plantar fasciitis can be debilitating, and it is strongly suggested that you are under the care of a podiatrist if you are experiencing heel pain.
The pain and discomfort that is found in plantar fasciitis is located in the heel and arch area of the foot. It develops as a result of inflammation that affects the plantar fascia. The plantar fascia is a band of tissue that connects the heel to the toes and runs along the bottom of the foot. The contributing factors for developing plantar fasciitis can include standing on hard surfaces for the majority of the day and wearing uncomfortable shoes, such as high heels. Additionally, patients who have gained weight may develop this ailment, and it can affect people who have low or high arches. The pain that accompanies plantar fasciitis can be debilitating, and it is strongly suggested that you are under the care of a podiatrist if you are experiencing heel pain.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Roy Rothman, DPM from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
How Can It Be Treated?
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our office located in DeBary, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
 Arthritis is a common disease that affects the joints of a person’s body, including the joints of the feet. The severity of a person’s arthritis can vary, however most patients complain of a painful stiffness that they experience in their joints. Other common symptoms may include redness and swelling of the skin where the joints are feeling stiff and sore. Some patients have also expressed that they have difficulty walking and lack mobility and flexibility in their joints. For a proper diagnosis and advice on how to best treat arthritis in the feet and ankles, please speak with a podiatrist.
Arthritis is a common disease that affects the joints of a person’s body, including the joints of the feet. The severity of a person’s arthritis can vary, however most patients complain of a painful stiffness that they experience in their joints. Other common symptoms may include redness and swelling of the skin where the joints are feeling stiff and sore. Some patients have also expressed that they have difficulty walking and lack mobility and flexibility in their joints. For a proper diagnosis and advice on how to best treat arthritis in the feet and ankles, please speak with a podiatrist.
Arthritis can be a difficult condition to live with. If you are seeking treatment, contact Roy Rothman, DPM from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Arthritic Foot Care
Arthritis is a joint disorder that involves the inflammation of different joints in your body, such as those in your feet. Arthritis is often caused by a degenerative joint disease and causes mild to severe pain in all affected areas. In addition to this, swelling and stiffness in the affected joints can also be a common symptom of arthritis.
In many cases, wearing ill-fitting shoes can worsen the effects and pain of arthritis. Wearing shoes that have a lower heel and extra room can help your feet feel more comfortable. In cases of rheumatoid arthritis, the arch in your foot may become problematic. Buying shoes with proper arch support that contour to your feet can help immensely.
Alleviating Arthritic Pain
It is best to see your doctor for the treatment that is right for your needs and symptoms. Conditions vary, and a podiatrist can help you determine the right method of care for your feet.
If you have any questions, please feel free to contact our office located in DeBary, FL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Arthritis is an inflammation of the joints and it can occur at any joint in the body, especially in the foot. It generally effects those who are older, however, it can occur at any age. Although there are many different forms of arthritis, there are three main types that occur in the foot. The three types are osteoarthritis, rheumatoid arthritis, and gout.
The primary cause of osteoarthritis is aging. As you age, cartilage degenerates around the joints which causes friction and pain. Obesity can cause osteoarthritis through mechanical stress. Injuries that damage joints can increase the probability as well. Finally, a family history of osteoarthritis can also increase chances of having it.
Rheumatoid arthritis occurs when the immune system attacks the joint linings and weakens them over a long time. While there is no known cause of rheumatoid arthritis, obesity and smoking can increase your chances of getting it. Women are also more likely to get it than men.
Gout is a form of arthritis that occurs when there is too much uric acid in your blood and painful crystals form in your joints. Men are more likely to have gout than women. People who are obese or drink alcohol often are also more likely to develop gout. Furthermore, having diabetes, heart disease, high blood pressure, high cholesterol, gastric bypass surgery or a family history of gout may increase your likelihood of developing the condition.
Symptoms of arthritis include pain, stiffness, swelling in the joints. These symptoms can make it harder and more painful to walk. Physical activity can increase pain and discomfort. Furthermore, joint pain can worsen throughout the day for osteoarthritis. Gout attacks generally last several days with the first few being the worst.
Diagnosis of gout includes either a joint fluid test or a blood test. X-ray imaging can detect osteoarthritis but not gout. On the other hand, there is no blood test for osteoarthritis. Rheumatoid arthritis is difficult to diagnosis. Doctors utilize family and personal medical history, a physical examination, and antibody blood tests to determine if you have rheumatoid arthritis.
Treatment varies for the different kinds of arthritis. Anti-inflammatory medication or steroids can help reduce pain from inflammation of the joints. Changing shoe types can help with some symptoms. Wider shoes can help with discomfort from gout and osteoarthritis. High heels should be avoided. Shoes with proper arch support and that take pressure off the ball of the foot can help with rheumatoid arthritis. Drinking lots of water can also help rid uric acid from the blood. Losing weight, improving your diet, and limiting alcohol and smoking can also help prevent or lessen the symptoms of arthritis.
If you are having trouble walking or pain in your feet, see a podiatrist to check if you have arthritis.